
The realms of disease and illness are full of acronyms… ALS, CF, COPD, DS, GERD… The list goes on and on. A few that you’ve probably never heard of, at least until you or a loved one have had them applied to you… Are I.L.D, P.F, I.P.F, and non-I.P.F.
Lets start off with I.L.D. This is not a disease in and of itself. Rather its a grouping of them. I.L.D stands for Interstitial lung disease. An umbrella term for a large group of disorders. That cause scarring in a person’s lung tissue.
The word “interstitial” refers to the space between objects. The “space” involved with an Interstitial Lung Disease (I.L.D) is found between the working bits and pieces of the lungs. For instance there is space between the lung’s air sacks (Alveoli) and the blood vessels. But this space isn’t an empty void. It contains connective tissue. This “in between” tissue… is “interstitial” tissue. Or as it is also referred to, the “interstitium.”
So simply put, an “Interstitial Lung Disease” is a disease that effects the connective (in between) tissue of a patient’s lungs.
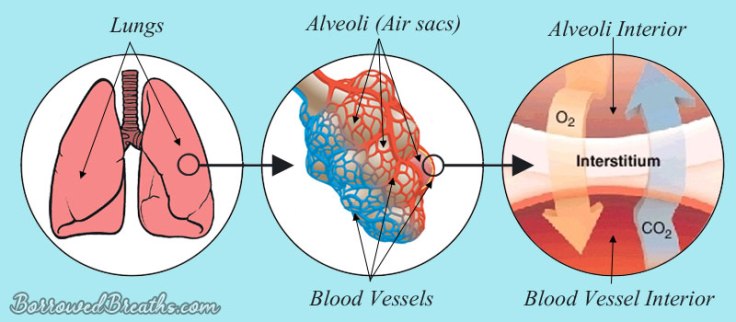
When the interstitial tissue becomes damaged, whether the cause is known or unknown, and scar tissue forms… it is PF. Which stands for Pulmonary Fibrosis. Pulmonary refers to anything having to do with the lungs. While fibrosis means scaring. So pulmonary fibrosis is just the medical term for scarring of the lungs.
You may also hear this condition referred to as “honeycombing” or “honeycomb lung.” The reason for this is that the scarring can resemble the honeycombs made by bees. Not the perfect hexagons bee keepers use on honey farms. But rather the natural haphazard product of bees out in the wild.

Pulmonary Fibrosis (PF) gets subdivided into two classifications based on whether or not an underlying cause is know. The most common type being Idiopathic Pulmonary Fibrosis (I.P.F). Idiopathic refers to something that has an unknown cause… So “Idiopathic Pulmonary Fibrosis” is the medical term for Scarring of the lungs without a known underlying cause.
I.P.F is what I was diagnosed with after honeycombing was discovered in my lungs and no definitive cause could be determined. If the cause had ever been discovered, then my diagnoses would have been changed.
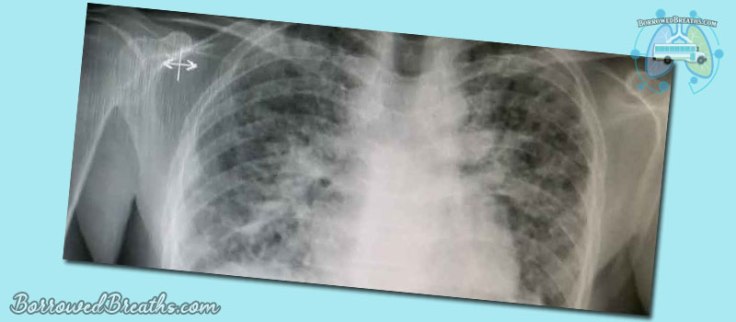
When the underlying cause is known… then a patient is diagnosed with non-Idiopathic Pulmonary Fibrosis (non-I.P.F). Though defining “non-Idiopathic” is a little confusing because it requires the use of a double negative.
Since “idiopathic” means the cause is unknown. “Non-Idiopathic” means the cause is NOT unknown. Or more simply put… “non-Idiopathic” means that the cause IS known.
This can get extra confusing. Because “non-idiopathic” and “non-I.P.F” are not the phrases commonly used in everyday conversation to denote non-Idiopathic Pulmonary Fibrosis. More often you will simply hear “Pulmonary Fibrosis” or “P.F” used.
However; I.P.F and non-I.P.F are both Pulmonary Fibrosis.

Pulmonary fibrosis is a progressive chronic disease. Meaning that over time the scarring it creates… worsens. Causing stiffness in the lungs and making it more difficult to breathe. The damage caused to the lungs by this scarring is irreversible. Sadly there is no cure and no way for the lungs to heal.
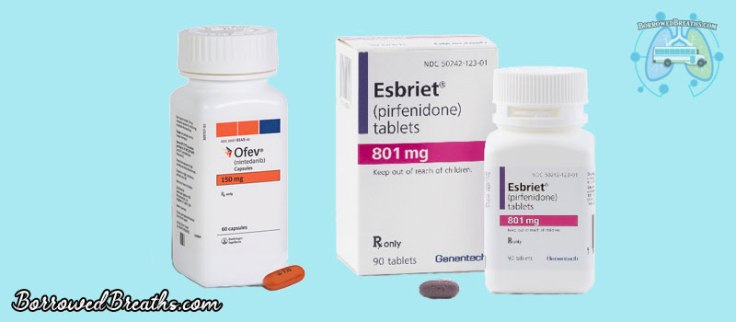
Though in some cases, it’s progression can be slowed by medications… Prolonging a patients life. Ofev and Esbriet being the two most commonly prescribed for Idiopathic Pulmonary Fibrosis (I.P.F). While any medication prescribed for non-I.P.F will vary depending on the underlying cause.
Rheumatoid arthritis and GastroEsophageal Reflux Disease (GERD) for example… can both lead to fibrosis developing in a patients lungs. But their treatments require different types of medication.
Eventually, regardless of the cause of the fibrosis, patients will find themselves in need of supplemental oxygen. The amount required can vary from person to person. But as time passes patients will find that they are in need of more and more.
For some this change will be gradual. Perhaps never becoming to big of a hindrance to their daily lives. For others this change may be rather rapid and/or dramatic. There is no set pattern of progression and it varies from patient to patient.
When I was first prescribed supplemental oxygen I needed a continuous flow at a rate of about three liters per minute (3lpm). By the time I was hospitalized I was using 15lpm. And once I was in the hospital I was on 100% pure O2 at 60lpm.

While there is no cure, some people with Pulmonary fibrosis (P.F.) can be eligible for lung transplants. This can be a difficult choice for some however. Because they are essentially deciding on whether or not to trade one illness… for another. Scarring in the lungs for a weakened immune system that wants to destroy their new lungs.
For me the choice was to have a transplant. I was still relatively young and my quality of life was virtually non existent. Pre-hospitalization my world encompassed my home and pulmonary rehab. With hospitalization my world shrunk to a hospital bed and walks around the ward. Given the opportunity the decision to risk a transplant was an easy one.
However; I know others who’s situation hasn’t been as dire as my own. Folks who still manage to have an enjoyable quality of life, who are older, and who… wishing to let others have the chance at the opportunity of a better life. Have opted not to pursue a transplant. While there are some patients who, even though they might benefit from a transplant. Have weighed the pros and cons against the risk… and decided it’s not the right choice for them.

Pulmonary fibrosis, be it idiopathic or non-idiopathic, can be overwhelming and terrifying. Especially once you start delving into what the internet has to say on the topic. That, followed by trying to navigate which treatment path to pursue and… well lets just say I am not surprised by the number of folks out there who feel defeated before they’ve even started.
That doesn’t have to be one’s final mindset however.
Anyone suffering from pulmonary fibrosis or who has a loved one suffering with pulmonary fibrosis… learn as much as you can from reputable sources, try not to freak out from the negative articles you’ll read online, find a doctor you like, trust, and who specializes in Interstitial Lung Diseases. And as difficult as it may seem…. stay positive and be tenacious.
